Health News
Get Health News and Updates
Health News
Get Health News and Updates

Find a Doctor
We have expert providers for all your health needs
Find a Location
Get care close to where you live or work
Patients & Visitors
Get helpful information to make the most of your visit.
Pay a Bill
Make a secure online payment for your hospital and physician bill
Patient Portal
Sign in to your account and take care of your healthcare needs.

Our Locations
With hospitals and urgent care centers to physician offices throughout Northern New Jersey, you can get care close to where you live or work.
St. Joseph’s University Medical Center
St. Joseph’s Wayne Medical Center
St. Joseph’s Totowa Health Campus
St. Joseph’s Children’s Hospital
The Cancer Center at Totowa
St. Jospeh’s Urgent Care
St. Joseph’s Health Physical Rehabilitation
St. Joseph’s Health Imaging
Expert Doctors. Convenient Care.
We have leading primary care physicians and specialists in nearly every field of medicine. Get care when and where you need it.
- Same-day, early, late, and weekend appointments
- Video visits offered
- Most insurance plans accepted

Latest News & Health Tips


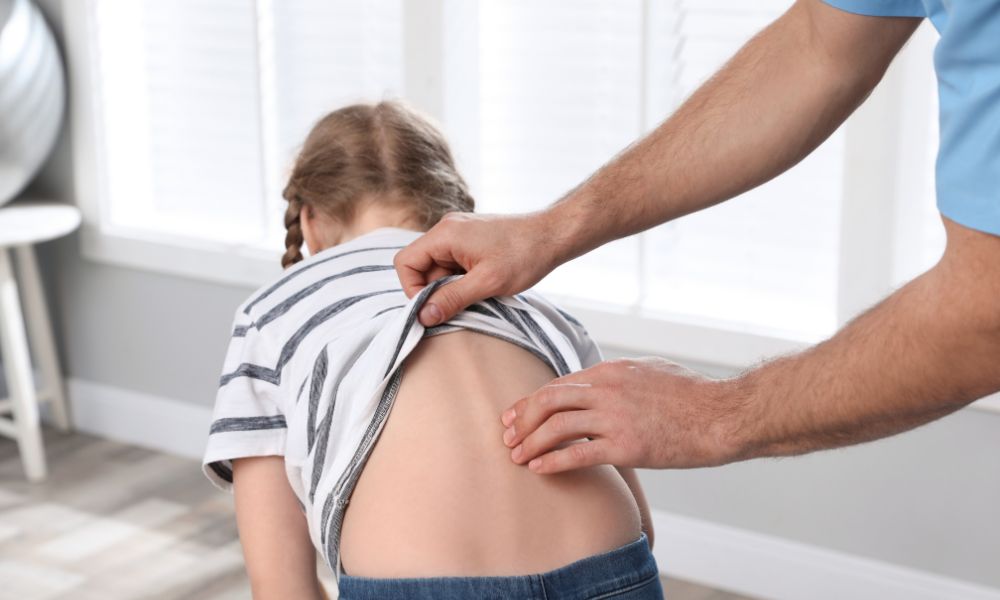
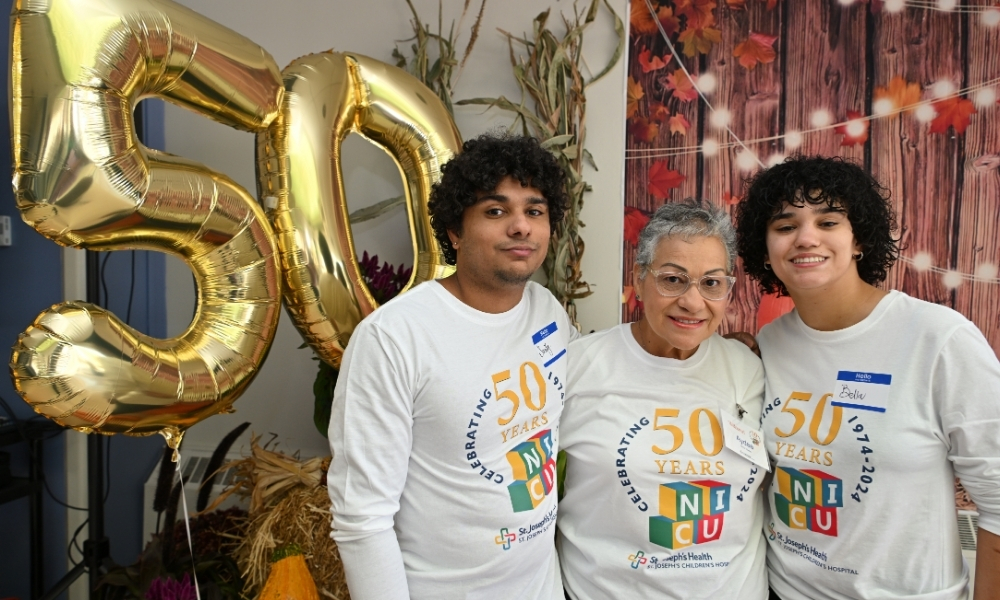

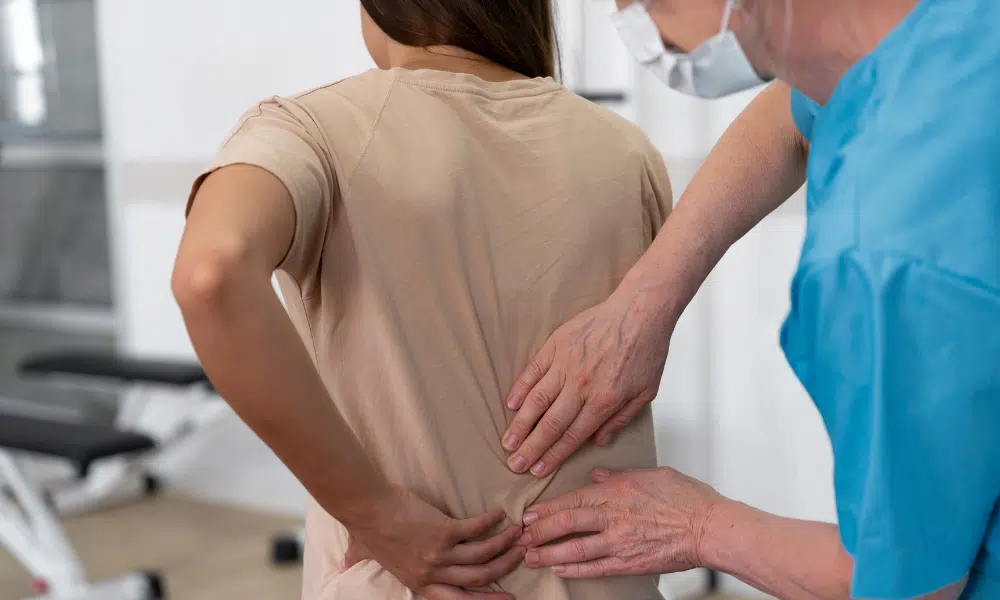




Awards and Accreditations














Get the Latest Health and Wellness News
Subscribe to receive health information from St. Joseph’s Health experts delivered straight to your inbox.





